A world where all births are safe
We are a global research program for saving lives at birth.
From donorship to ownership
Safer Births received funding from the Global Financing Facility under the World Bank to scale up to 30 hospitals in Tanzania. Based on the promising results, it will in the next phase scale up to 100+ hospitals. Watch the video to learn more.

May 2023 Update
The Safer Births Bundle of Care May 2023 Update summarizes the history, implementation, and learnings from the project so far.
It also outlines the promising preliminary results and the estimated cost-effectiveness over time.
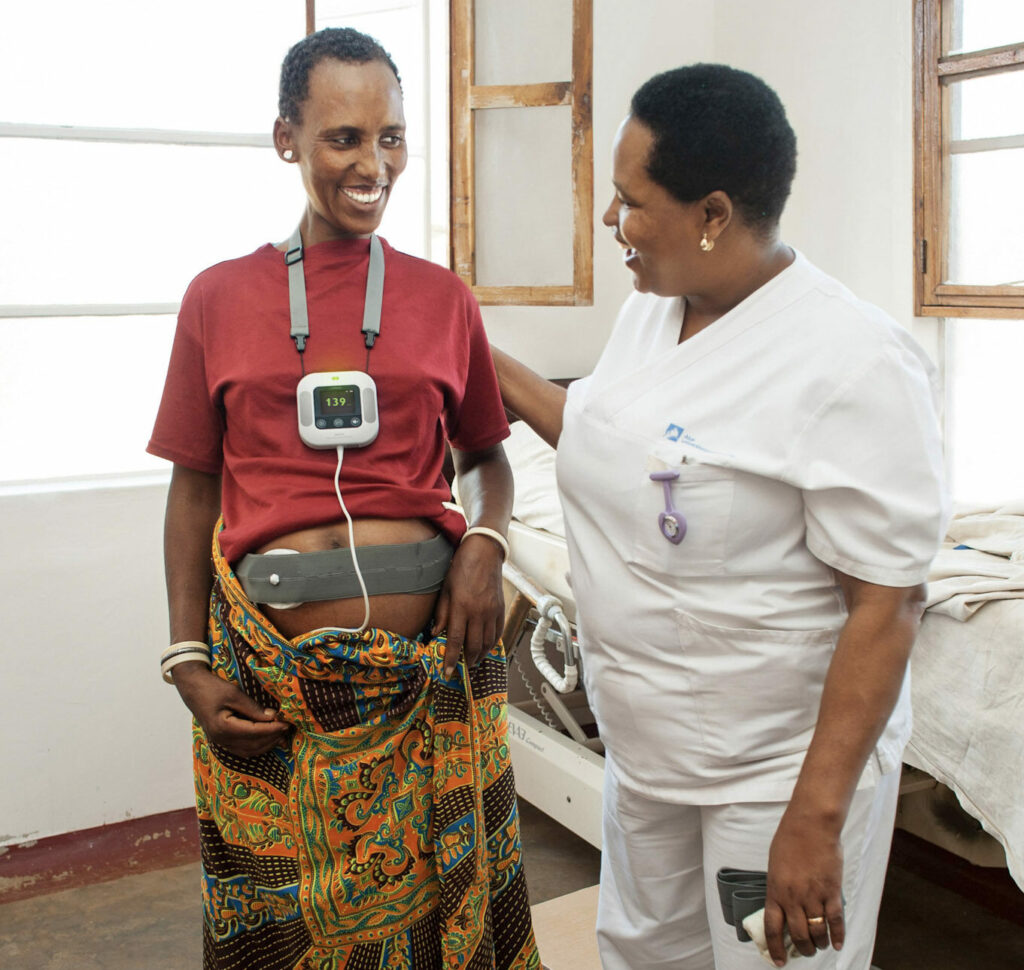
Reducing maternal deaths
Globally bleeding after birth is a leading cause of maternal deaths.
The Safer Births Bundle of Care program trains healthcare professionals to efficiently deal with PPH and is already resulting in up to a 50% decrease in maternal deaths.
Watch the video to learn more.
Creating a culture of trust and quality improvement
In Tanzania the Safer Births Bundle of Care program is helping reduce maternal and newborn mortality.
It is also changing the way people work, with weekly simulation training, and debriefing, and the use of data for quality improvement.
Watch the video to learn more.
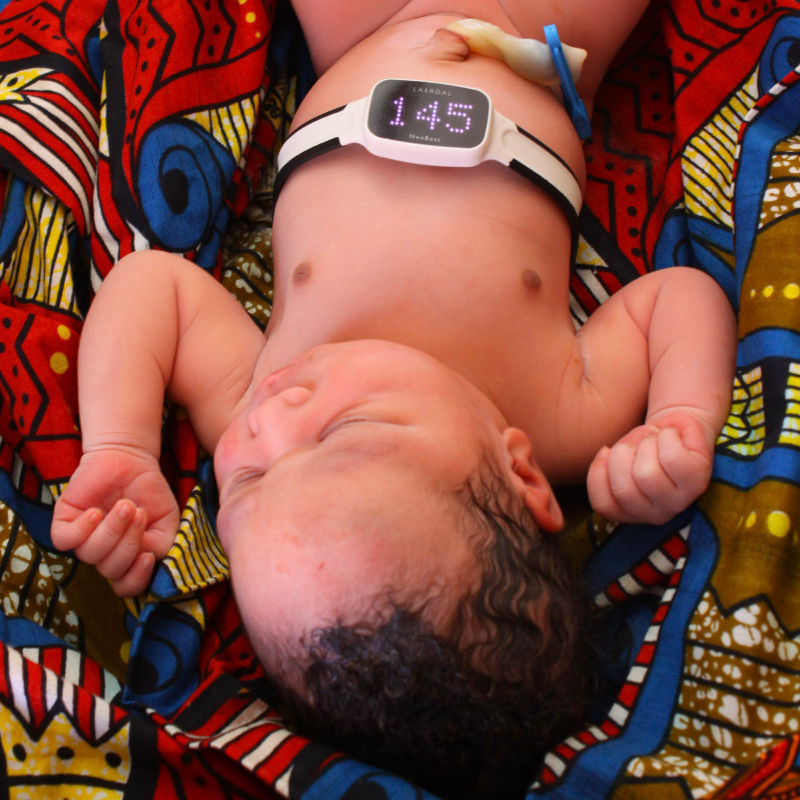
Research: A journey to safer births
Evidence-based innovations
The Safer Births Innovations enable healthcare providers to make time-critical lifesaving decisions on the spot. The Safer Births Bundle of Care is a collection of training and clinical tools to help prevent and treat the leading causes of newborn and maternal death.